Overuse, injury, and diseases are fairly common problems that damage our joints, making them prone to degeneration. So, it’s only natural to wonder: how to overturn this? What helps rebuild cartilage in the knees?
Well, with the advancement of medicine, several surgical procedures can help with this. Certain dietary supplements may promote cartilage health as well.
But to understand what they are and how they work, you need to know why it’s so challenging for cartilage to regenerate on its own first. Here’s what we’ll cover, tap on any of these bullets to easily navigate through the article:
- Why it’s hard to naturally repair cartilage
- 4 surgical procedures to heal cartilage
- Am I a good candidate for cartilage repair?
- Supplements that promote cartilage health
- FAQs
Let’s get started!
Why is it so hard for the damaged knee cartilage to repair itself?
Cartilage is the main type of connective tissue throughout the body. It is an important structural component of the joints, and there are three types of it (1):
- Hyaline.
- Elastic.
- Fibrocartilage.
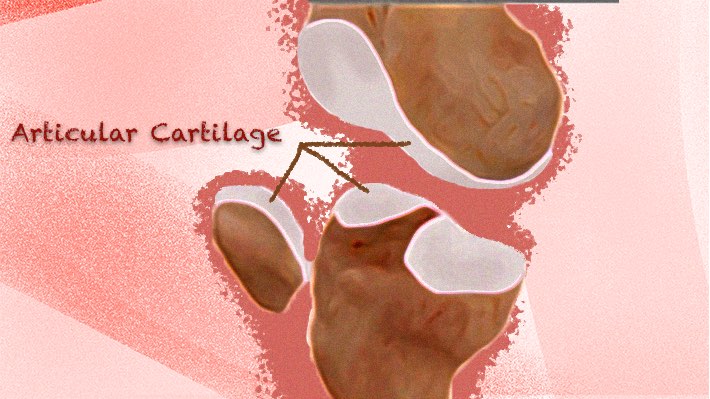
The hyaline cartilage, found at the ends of the bones, is the one we’ll focus on for this article. It works as a shock absorber, making sure the joints can move smoothly. It’s also the one that deteriorates in wear and tear. (1)
Hyaline cartilage has limited potential to heal.
This is due to two main problems – lack of blood supply and the speed of the cartilage regeneration process.
See, healing and growth rely on circulation – blood brings nutrients to the injured area so it can repair itself. But cartilage doesn’t have blood vessels, thus making it way more challenging for it to recover. (1, 2)
Apart from that, this tissue takes a long time to grow new healthy cartilage cells. The unrepaired tissue can in turn increase friction inside the joint, worsening the damage. (3)
Learn more: The cartilage degeneration process for dummies.
4 procedures to heal damaged knee cartilage
Due to its limited potential to heal, cartilage may need some external help to repair and restore itself.
This is usually done through surgery, but the procedure itself will depend on the patient and the level of damage. Common surgical techniques include (4):
1) Bone marrow stimulation procedure
Arthroscopic bone marrow stimulation is the first line of treatment for cartilage regeneration, mostly because it preserves the integrity of your knees. (5)
To do it, your surgeon removes the damaged tissues with an arthroscope. Then, the physician will make minor cuts and abrasions to the underlying bone. Doing this helps bring blood and repair tissues to the injury site, stimulating healing. (5)
It is a minimally invasive and cost-effective procedure. However, it is not without some drawbacks, which include (6):
- Abnormal bone growth.
- Increased risk of osteoarthritis.
- Poor knee functioning.
2) Mosaicplasty
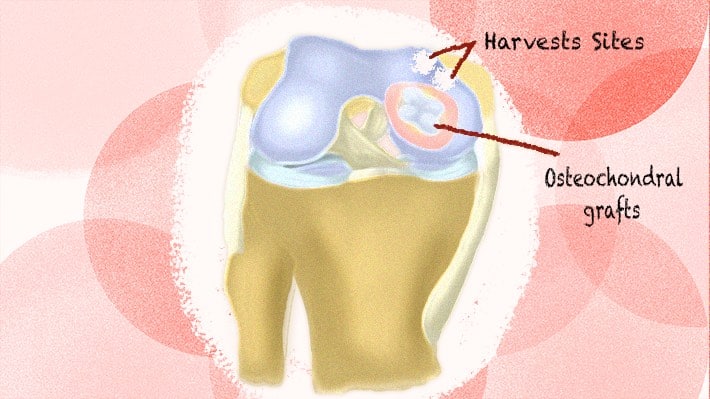
Also known as “osteochondral transplantation technique”, mosaicplasty involves the repair of cartilage and bone lesions. It’s done by harvesting healthy, undamaged tissues from one place and placing them in the damaged area. (7, 8)
The site for extraction is usually another weight-bearing joint, like the femur. The harvested tissue is then inserted into the defective sites by drilling holes either through open surgery or with an arthroscope. (7, 8)
The transplanted tissue improves the durability of the knee joint. While it can repair large areas of damaged cartilage, it cannot be performed if you have the following (7, 8):
- Osteoarthritis.
- Rheumatoid arthritis.
- Infection.
- Tumor.
3) Autologous chondrocyte implantation (ACI)
ACI is one of the most widely used techniques for the treatment of large areas of cartilage damage.
The surgical procedure involves collecting your healthy cartilage cells to grow them in a laboratory. Then, they are surgically reimplanted into the damaged tissue.
The drawback of this procedure is that it takes a significant amount of time and money. (7)
4) Stem cell therapy
Stem cells are the body’s raw material from which all the other cells can be regrown, including the cartilage. This makes them a very promising source for repairing cartilage lesions.
After extracting the stem cells, your surgeon inserts them into the knee through a surgical incision. Once in there, they can theoretically transform into new cartilage cells.
Although stem cell therapy may improve cartilage health, the biggest drawback is that the cells can potentially migrate to other sites, causing unwanted cartilage growth. (9)
Am I a good candidate for knee cartilage repair?
Although surgeries for cartilage repair are increasingly performed, they are not suitable for everyone. You are a good candidate for these procedures if you (7, 10):
- Are younger than 40 years.
- Experience knee pain at rest.
- Are active.
- Have had pain for a few months (not years).
- Have localized cartilage damage (one or two isolated injuries to the cartilage).
- Do not have problems with knee stability or alignment.
- Have healthy ligaments.
Otherwise, the surgery may not succeed. If you are not eligible for these procedures, there are other ones available, like knee joint replacement.
Supplements that promote cartilage health
Some supplements may help the cartilage heal, whether by reducing inflammation or by giving it building blocks to repair itself.
They are an interesting option for those wanting to maintain healthy knees, or that can’t undergo surgery for any reason.
Now, the supplements that have some evidence supporting their benefits on cartilage include (11, 12):
Related: Best supplements for knee cartilage health.
FAQs
How to rebuild cartilage in the knee naturally?
By exercising, having a healthy lifestyle, and sleeping well. You can also boost this with supplements like glucosamine and chondroitin.
Conclusion: How do you rebuild cartilage in your knees?
Knee damage can negatively impact your day-to-day functioning. While it is difficult for this tissue to regenerate by itself, several cartilage repair procedures can help you regain your mobility and ease joint pain.
This can be done with one of many types of orthopaedic surgery. Such as:
- Bone marrow stimulation.
- Osteochondral transplantation technique.
- Autologous chondrocyte implantation.
- Stem cell therapy.
Some supplements may also help if your knee osteoarthritis is causing pain. However, it’s best to check with your doctor to learn the best treatment options.
Resources
- Chang LR, Marston G, Martin A. Anatomy, Cartilage. [Updated 2021 Oct 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532964/
- Vangsness, C Thomas Jr et al. “Restoring articular cartilage in the knee.” American journal of orthopedics (Belle Mead, N.J.) vol. 33,2 Suppl (2004): 29-34.
- Hayes, D W Jr et al. “Articular cartilage. Anatomy, injury, and repair.” Clinics in podiatric medicine and surgery vol. 18,1 (2001): 35-53.
- Feucht, Matthias J et al. “Stellenwert der chirurgischen Knorpeltherapie bei Früharthrose” [Cartilage repair procedures for early osteoarthritis]. Der Orthopade vol. 50,5 (2021): 356-365.
- Murawski, Christopher D et al. “A Review of Arthroscopic Bone Marrow Stimulation Techniques of the Talus: The Good, the Bad, and the Causes for Concern.” Cartilage vol. 1,2 (2010): 137-44.
- Hoffman, James K et al. “Articular cartilage repair using marrow stimulation augmented with a viable chondral allograft: 9-month postoperative histological evaluation.” Case reports in orthopedics vol. 2015 (2015): 617365.
- Rönn, Karolin et al. “Current surgical treatment of knee osteoarthritis.” Arthritis vol. 2011 (2011): 454873.
- Oztürk, Alpaslan et al. “Osteochondral autografting (mosaicplasty) in grade IV cartilage defects in the knee joint: 2- to 7-year results.”International orthopedics vol. 30,3 (2006): 200-4.
- Liu, Yanxi et al. “Strategies for Articular Cartilage Repair and Regeneration.” Frontiers in bioengineering and biotechnology vol. 9 770655. 17 Dec. 2021.
- Sharma, AK. “Campbell’s Operative Orthopaedics.” Medical Journal, Armed Forces India vol. 60,1 (2004): 91.
- Henrotin, Yves, and Ali Mobasheri. “Natural Products for Promoting Joint Health and Managing Osteoarthritis.” Current rheumatology reports vol. 20,11 72. 19 Sep. 2018,
- Thomas, Sally et al. “What is the evidence for a role for diet and nutrition in osteoarthritis?.” Rheumatology (Oxford, England) vol. 57,suppl_4 (2018): iv61-iv74.



