
Cartilage degeneration can happen on any knee joint surface. When it’s behind the patella, it’s called “osteoarthritis in knee cap” or “chondromalacia patella.”
This is extremely common – at least half of people with anterior knee pain have some degree of it. (1) The good news is that most patients will have a full recovery with the right treatment. (2)
We’ll discuss all about this condition below – from its causes to the best treatments. Here’s what you’ll learn, tap on any of these topics to navigate through the article:
What is osteoarthritis in the kneecap?
Knee osteoarthritis is a condition that happens when the articular cartilage of this joint degenerates. When it affects the patella -the bone at the front of the knee-, there’s kneecap osteoarthritis.
This type of osteoarthritis is also called patellofemoral arthritis and chondromalacia patella. People with this diagnosis may have degenerative changes on the kneecap only, or in other areas of the joint as well. (1)
Side note: Cartilage degeneration can happen in any joint, but the knee is one of the most commonly affected. Joints with a weight-bearing role like the knee or the hip tend to be prone to cartilage damage.
Causes of patellar osteoarthritis
The two main causes of kneecap OA are (1):
- Malalignment. The patella doesn’t glide properly, which can increase the pressure in specific areas of the cartilage, wearing them down.
- Kneecap fracture. This injury can cause direct damage to the cartilage.
Related: Can you walk with a kneecap fracture?
This condition has several risk factors.
These are situations or conditions that can make you prone to developing osteoarthritis on the kneecap. The most common include (1, 2):
- Medical history of kneecap instability, dislocation, or subluxation.
- Participating in running sports.
- People that have to climb stairs and/or kneel frequently.
- Having an ACL ligament injury repaired with either a hamstring or patella tendon graft.
- Being a woman.
- Having obesity.
- Having rheumatoid arthritis or other systemic disorders.
Symptoms of patellofemoral knee arthritis
The most common symptom is knee pain at the front of the joint. It tends to worsen after going up or downstairs, standing up, sitting down, and kneeling. (1)
Specific exercises like squats and lunges can also increase pain. However, these symptoms rarely affect the entire knee. (1)
Other symptoms include (1):
- Crepitus – knee popping, cracking, or grinding.
- Feeling like the knee gets locked.
- A sensation of instability or like the joint gives away.
- Swelling and/or tenderness around the kneecap.
Now, crepitus isn’t always a sign of patellar osteoarthritis. In fact, it’s extremely common and benign if it happens in isolation.
Learn more: 3 harmless reasons why knees crack and when to worry about it.
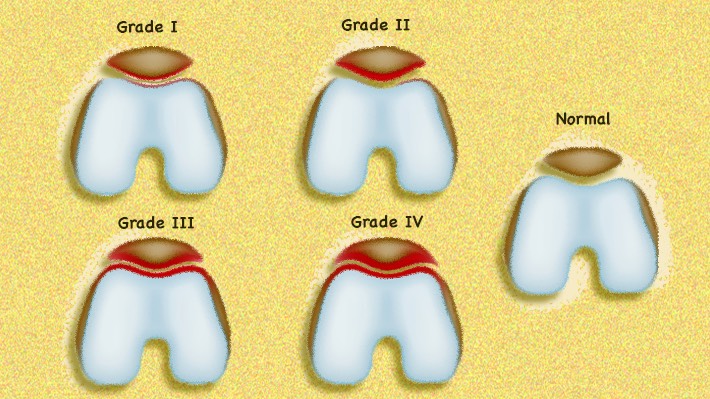
Diagnosis of chondromalacia
To diagnose this condition, the doctor will first perform a physical exam. He/she will assess your knee and do a series of movement tests to check your symptoms.
Then, the physician will do a medical interview. She/he will ask for your symptoms, any previous medical conditions, knee injuries, and family history, among other things.
Finally, the doctor will request imaging tests, usually x-rays. The presence of bone spurs, lack of joint space, or reduction of joint fluid are indicative of kneecap osteoarthritis. (1)
All this process is to rule out other conditions, like (1):
- Knee osteoarthritis in other parts of the joint.
- Iliotibial band syndrome.
- Patellar tendonitis.
- A disc herniation.
- Gout or pseudogout.
- Infection.
- Rheumatoid or psoriatic arthritis.
Treatment for patellofemoral joint osteoarthritis
The treatment of knee osteoarthritis is a bit challenging. See, there’s no therapy yet that can regenerate the lost cartilage.
That’s why the treatment options focus on managing symptoms and preventing the knee cartilage damage from getting worse.
With that said, most people do get better and achieve a full recovery after treatment.
This timeline varies widely from person to person, though – it can take from 1 month to a few years. (2)
Also, the type of treatment highly depends on the person. For example, younger patients may recover with conservative treatments alone. But older patients may need injections or surgery to manage symptoms. (1)
Now, the recommended treatments for patellofemoral joint osteoarthritis include:
1) Physical therapy
This is a mainstay in any knee osteoarthritis treatment plan. Physios are healthcare providers trained to treat joint problems and help you get back on track.
We do it through a customized treatment according to your symptoms, age, lifestyle, and goals. In a nutshell, your therapist will help you:
- Correct the patella maltracking – if any.
- Strengthen your quadriceps muscles to protect the kneecap cartilage from damage.
- Reduce your pain and swelling through a variety of therapies – heat, cold, massage, manual techniques…
- Teach you how to work with osteoarthritis.
- Give you any other strategy you may need to recover.
If you have post-traumatic arthritis, your physio will help you recover from the root injury as well. This will prevent patellar arthritis from worsening.
2) Wear a knee brace
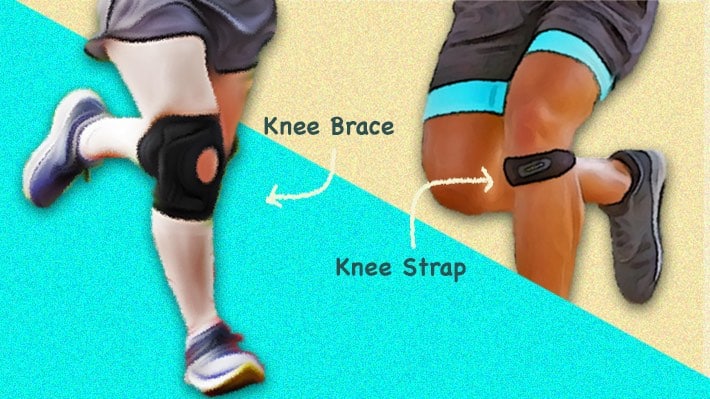
These garments can be very effective at reducing knee joint pain from patellar osteoarthritis. (1, 3) They can help you in your daily living, making it easier to climb stairs, exercise, or do your usual activities.
Yet, there are thousands of designs available – it’s key to find the right one for your needs. Now, the best knee braces for patellofemoral joint osteoarthritis include (1):
Knee sleeves
These work by compressing the knee joint, which in turn keeps it warm due to the increased blood flow. This in turn can reduce pain and stiffness.
Some models are completely closed, while others have a hole for the kneecap. This can be helpful for patellar osteoarthritis, as it can reduce the pressure on the area.
These could help:
Patella stabilizing braces
If you have patellar maltracking, or if your kneecap tends to go out of place frequently, try one of these. They have a kneecap buttress that helps keep this bone in place during your activities.
Check this out: Best knee braces for patellar dislocation.
Patellar straps
These are minimalistic garments that apply direct pressure to the patellar tendon. This reduces the stress on the kneecap as a result, alleviating symptoms.
This can help: Our top picks of patella straps.
3) Home remedies
These are key to helping you manage your knee joint pain. Your therapist will likely suggest a series of home treatments for your specific symptoms, but these are the most common:
- Applying a hot or ice pack to the affected patellofemoral joint.
- Doing specific stretching or strengthening exercises.
- Massaging your thigh bone muscles to reduce the pressure on the kneecap.
- Losing weight to decrease the pressure on the kneecap.
- Using a transcutaneous electrical nerve stimulation (TENS) device to control pain.
This can help: 11 home treatments for knee joint OA (that work).
4) Activity modification
Changing the way you do certain activities is key to helping you reduce pain and heal. This is extremely individual, though – the best person to help you with this is your therapist.
For example, if you do regular exercise, talk with your physio about modifications you can try to not make your symptoms worse. This can look like not doing squats for a while and working on the quad machine instead, for example.
5) Dietary supplements
Taking certain dietary supplements can help with knee pain. However, it’s true that some people feel benefits, while others don’t. (3)
We think they’re worth a try, though. Most have practically no side effects -unlike NSAIDs- and can be taken by people with other health conditions. (3)
Common supplements for knee osteoarthritis include:
Learn more: Complete guide with supplements for knee OA.
6) Medication
Anti-inflammatory drugs like NSAIDs provide quick pain relief. As such, they’re recommended for people going through a flare-up. It’s not a good idea to take them for the long term due to their side effects. (3)
Another option is steroid injections.
Here, the doctor injects corticosteroid into the synovial fluid. This also relieves knee pain fairly quickly. These should be done in specific cases because there’s a risk of accelerating osteoarthritis. (3)
There are also hyaluronic acid injections, creams, and dozens of other drugs available for this condition. That’s why we made an evidence-based guide with the top 11 medicines for knee OA.
7) Surgery
Surgical intervention is the last resort for patellofemoral arthritis, and for a small number of patients. (1)
Your doctor may discuss surgical options if you’ve been doing at least 6 months of conservative treatments with absolutely no improvement. (4)
The type of surgery will entirely depend on the patient – age, symptoms, lifestyle… And the person must do physical therapy afterward to ensure a full recovery.
Now, common surgeries for this condition include (2):
- Chondroplasty.
- Arthroscopy.
- Patellar realignment.
- Patellofemoral replacement.
- Total knee replacement.
This may help: When is time for knee osteoarthritis surgery?
FAQs
What does arthritis in the kneecap feel like?
It causes pain in the front of the knee that often worsens when walking, climbing stairs, or standing up.
How do you treat arthritis in the knee cap?
This highly depends on the person. Most people without previous medical conditions will improve with physical therapy, home treatments, activity modification, and medication.
Is walking bad for knee osteoarthritis?
On the contrary, it’s excellent for this condition. Studies suggest that walking +6000 steps daily can ease symptoms and protect the knee from further deterioration. (5)
But first, discuss it with your physio. You may need additional recommendations to get to those daily steps without making your symptoms worse.
Conclusion: Osteoarthritis under knee cap
Patellar osteoarthritis is a fairly common condition. It usually comes with anterior knee pain and crepitus.
Most of the time is a consequence of other issues – like a previous injury, or rheumatoid arthritis. But it does get better with treatment.
Now, the treatment strategies for patellofemoral arthritis will depend on the person. We hope this guide helped you learn about your options and decide which ones can work for you.
Finally, when in doubt, talk with your physical therapist. We’re here to help you!
Resources
- Kiel J, Kaiser K. Patellofemoral Arthritis. [Updated 2021 Jul 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK513242/
- Habusta SF, Coffey R, Ponnarasu S, et al. Chondromalacia Patella. [Updated 2021 Oct 21]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459195/
- American Academy of Orthopaedic Surgeons Management of Osteoarthritis of the Knee (Non-Arthroplasty) Evidence-Based Clinical Practice Guideline (3rd Edition). https://www.aaos.org/oak3cpg Published August 31, 2021
- Kim, Young-Mo, and Yong-Bum Joo. “Patellofemoral osteoarthritis.” Knee surgery & related research vol. 24,4 (2012): 193-200. DOI: 10.5792/ksrr.2012.24.4.193
- White, Daniel K et al. “Daily walking and the risk of incident functional limitation in knee osteoarthritis: an observational study.” Arthritis care & research vol. 66,9 (2014): 1328-36. DOI: 10.1002/acr.22362



