
“Primary osteoarthritis of the knee joint” is a medical term that describes the cause of wear and tear being the aging process. (1)
Secondary osteoarthritis, on the other hand, means that the degeneration happened faster due to something else. Like an injury or a medical condition, for example. (1)
Below, we’ll discuss all you need to know about primary knee OA – what causes it, who’s at risk, how to treat it, and more. Here’s what we’ll cover:
What is primary knee osteoarthritis?
It’s a term that points to the aging process as the cause of the degeneration of your knee joints. But to fully understand this, let’s recap what knee osteoarthritis is.
First, knee osteoarthritis is a degenerative joint disease where the cartilage wears off.
Cartilage is a soft tissue present on the surfaces of our joints. It cushions and protects them, letting our bones glide smoothly so we can move easily.
Now, the cartilage deteriorates constantly due to frequent use – this is known as cartilage breakdown.
But healthy bodies can counteract the cartilage breakdown process.
They can heal the broken cartilage to keep it healthy. But, there are 2 situations in which our bodies can’t restore the damaged cartilage:
First, during the aging process.
See, when we’re young, the regenerative abilities of our bodies are at their best. We can easily keep the balance between the rate of cartilage breakdown and regeneration.
But as we age, it gets more difficult for our bodies to regenerate the worn cartilage. We can’t counteract the rate of articular cartilage degeneration. At least not enough to keep healthy cartilage.
The joint degenerates as a result. That’s how a knee can develop primary osteoarthritis.
The second way is due to an injury or medical condition.
In this case, something else is increasing the rate of cartilage breakdown. It can be:
- A knee injury – like a meniscus tear or a knee sprain.
- A medical condition – like rheumatoid arthritis.
This is known as secondary osteoarthritis.
Learn more: All about secondary osteoarthritis in the knee
Risk factors of primary osteoarthritis of the knee
Some people are more prone to develop osteoarthritis than others. Now, the following can predispose someone to primary knee OA:
Sarcopenia
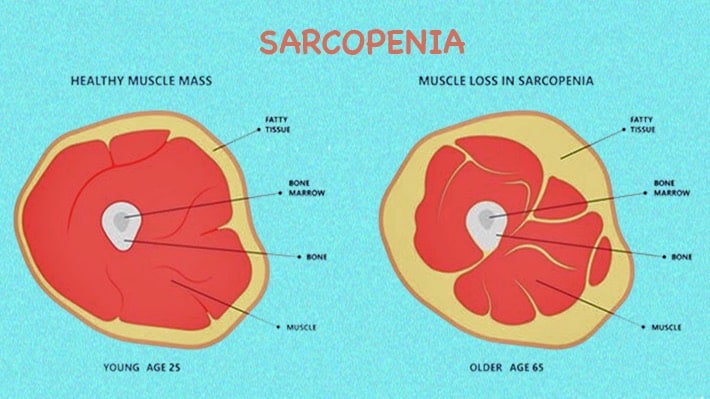
This is a common disease in the elderly, where the muscles lose strength and mass. This leads to weakness and, if severe, can reduce the ability to do daily activities. (2)
The problem here is that weak muscles promote primary knee osteoarthritis in 2 ways:
- They can’t protect the joint properly, which can speed up the rate of cartilage breakdown.
- They limit the amount of blood reaching the cartilage, impairing its regeneration.
That’s why muscle strengthening is a staple in knee osteoarthritis treatment. Strong knee muscles can protect the cartilage, promote healing, and delay the degenerative process.
Certain occupations
Jobs involving strenuous physical activity can make you prone to primary osteoarthritis. In particular, agricultural workers are most at risk. (3)
Having a congenital deformity
Certain deformities can make people prone to develop osteoarthritis. This is the case for people born with a valgus or varus deformity in the knees. (4)
This anatomic malalignment will inevitably change the way your knee joint distributes the weight. So, one side will be under more stress than the other, making it prone to unilateral wear and tear.
Being a female
Research shows that women are more at risk of developing osteoarthritis, perhaps due to a combination of factors. (3, 4)
One of them apparently is the differences in joint alignment. Having wider hips changes the angle of the thigh bone, which can increase the pressure on the knee joint. (4)
Another is going through menopause. This process causes several hormonal changes that affect the regenerative capabilities of cartilage. (4)
Symptoms of primary and secondary osteoarthritis
Contrary to popular belief, knee osteoarthritis doesn’t always show symptoms. (3, 5)
Some people are completely asymptomatic, while others develop debilitating knee OA symptoms. This only shows how complex this condition is. (5)
With that said, the people that have symptomatic knee osteoarthritis usually feel:
- Knee pain at varying degrees – from mild to severe.
- Joint stiffness – mostly after long periods of rest.
Now, if your doctor suspects knee osteoarthritis, he/she will likely request imaging tests.
This will show the current state of your knee joint. If there’s knee osteoarthritis, the X-rays or MRI will likely show:
- Abnormal articular cartilage.
- A reduction in joint space.
- Bone spurs.
Learn more: 10 symptoms of knee osteoarthritis
How to treat primary knee joint osteoarthritis
The treatment is the same as in secondary knee OA. It’s mostly focused on treating symptomatic osteoarthritis.
If done properly, some of these treatments may even slow the progression of the disease. The most common include:
Home treatment options
This type of knee arthritis is irreversible. That’s why it’s crucial you learn how to manage it at home.
The most common home treatments include:
- Using heat and cold therapies to relieve pain and joint inflammation.
- Following a home exercise program adapted to your needs to strengthen your muscles.
- Wearing a knee brace to make your daily activities easier and reduce pain.
- Taking over-the-counter medications like NSAIDs to keep pain flare-ups at bay.
Try this: 11 home treatments for knee osteoarthritis that work
Physical therapy
Rehabilitation is key in any knee OA treatment, regardless of its severity.
See, a physio is a healthcare provider trained to help you recover from joint and movement problems. As such, your therapist will:
- Teach you individualized strategies to manage your symptoms at home.
- Design a customized treatment plan to reduce joint swelling, pain, and other symptoms.
- Help you recover from surgery or other invasive treatments.
The best way to do this is by going to a physio in your area.
She/he will start with a physical examination and an interview. This is to learn more about your issues and goals, to tailor the plan to your needs.
Know more: Guide with everything about PT for osteoarthritis.
Dietary supplements
Several supplements can help with knee osteoarthritis pain. Some have anti-inflammatory properties, while others can promote the regeneration of damaged cartilage.
But in all honesty – these benefits aren’t immediate and they may not happen to everyone.
But dietary supplements are safe as long as you follow the manufacturer’s instructions, so they’re definitely worth a try.
The most common dietary supplements for knee joint osteoarthritis include:
Warning: Consult with your doctor before taking supplements if you’re taking other medications. Some supplements can interact with certain drugs – better be safe than sorry.
Injections
These are common treatments for managing symptoms or slowing down cartilage breakdown. Usual injections include:
Intra-articular corticosteroid injections
Corticosteroids are a type of drug that’s very efficient at reducing pain and swelling for up to 3 months. But, they may speed up the articular degeneration, so they should be used in specific cases. (6)
Hyaluronic acid
Hyaluronic acid is a chemical present in our joint fluid. Injecting it can help manage osteoarthritis symptoms for some people. (6)
Further reading: Ranking of the 15 best treatments of knee OA
Surgical treatment options

Surgery becomes the best option for joint pain relief if conservative treatment fails.
There are several surgical options available for knee osteoarthritis. But, as primary knee osteoarthritis is most common in the elderly, the surgical approaches available will likely be (7):
Partial knee replacement
This one is also known as “unicompartmental replacement.” It’s for patients with only one side of the knee joint affected with osteoarthritis.
In the procedure, orthopaedic surgeons replace the involved knee compartment with an artificial one.
Total knee replacement (TKR)
This procedure is the best treatment for severe knee osteoarthritis after all of the conservative and minimally invasive options have failed.
Yet, it’s imperative to make sure you actually need a total knee replacement. This is because studies show that up to 25% of people who underwent a TKR didn’t need it, which actually made their symptoms worse. (6)
FAQs
What is primary osteoarthritis of the knee?
It’s when knee osteoarthritis begins due to the aging process. There’s no other underlying cause other than that.
How is primary osteoarthritis treated?
Home treatments, NSAIDs, and physical therapy. In the final stages, most cases will need some kind of surgical management.
Is primary osteoarthritis a disability?
Legally speaking, it can be considered a disability if the symptoms are severe. Check with the Social Security Administration of your country to see if you’re eligible for disability benefits.
Conclusion: Primary knee osteoarthritis
Primary osteoarthritis mostly affects the elderly. It happens when no other diseases or injuries speed up the cartilage damage process.
Strong risk factors include sarcopenia-induced muscle weakness, being female, and physically demanding occupations.
There are several treatment options available. And, even though they won’t repair the cartilage damage, they can make sure you live as freely as possible and prevent pain and disability.
However, if your symptoms are severe, please consult with your physician. She/he will help you find the best treatment possible.
Resources
- Hsu H, Siwiec RM. Knee Osteoarthritis. [Updated 2021 Jul 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507884/
- Ardeljan AD, Hurezeanu R. Sarcopenia. [Updated 2021 Jul 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK560813/
- Rossignol, M et al. “Primary osteoarthritis and occupations: a national cross sectional survey of 10 412 symptomatic patients.” Occupational and environmental medicine vol. 60,11 (2003): 882-6. DOI: 10.1136/oem.60.11.882
- Aboulenain S, Saber AY. Primary Osteoarthritis. [Updated 2022 Feb 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557808/
- Culvenor, Adam G et al. “Prevalence of knee osteoarthritis features on magnetic resonance imaging in asymptomatic uninjured adults: a systematic review and meta-analysis.” British journal of sports medicine vol. 53,20 (2019): 1268-1278. DOI: 10.1136/bjsports-2018-099257
- The Royal Australian College of General Practitioners. Guideline for the management of knee and hip osteoarthritis. 2nd edn. East Melbourne, Vic: RACGP, 2018. Retrieved on March 2022 from: https://www.racgp.org.au/download/Documents/Guidelines/Musculoskeletal/guideline-for-the-management-of-knee-and-hip-oa-2nd-edition.pdf
- de l’Escalopier, Nicolas et al. “Surgical treatments for osteoarthritis.” Annals of physical and rehabilitation medicine vol. 59, 3 (2016): 227-233. DOI: 10.1016/j.rehab.2016.04.003
- “Osteoarthritis.” Arthritis Foundation. Retrieved on March, 2022 from: https://www.arthritis.org/diseases/osteoarthritis
- “Osteoarthritis.” National Institute of Arthritis and Musculoskeletal and Skin Diseases. Retrieved on March, 2022 from: https://www.niams.nih.gov/health-topics/osteoarthritis



